Value Based Payments
In Information Week David Carr writes about some of the current trends in health care, and especially about “value based payments.” He writes –
“Value based” is a catch-all label for Accountable Care Organizations (ACOs) and other ways of restructuring healthcare around payment for value delivered, as measured by metrics of healthcare quality or the aggregate health of a population rather than by the volume of visits, procedures, or hospital stays a healthcare organization records. In other words, it’s a highly data-driven vision of healthcare reform, intended to improve quality and efficiency while reducing costs.
He reports on a new study by Availity that says while 75% of providers currently participate in some form of “value-based payment model…fewer than 30% believe these schemes offer a good level of reward for the risk.” Generally, both physicians and hospitals are concerned about the additional administrative burden and expense needed to justify payment.
That concern is certainly borne out by an article titled “What is Value in Health Care?” from the New England Journal of Medicine sent to me by a friend. This was published in 2010 and written by Michael Porter of the Harvard Business School.
Porter is extremely well regarded, so what he writes must be taken seriously. But there is something about health care that makes even sensible people lose their grip. Porter starts off with –
In any field, improving performance and accountability depends on having a shared goal that unites the interests and activities of all stakeholders.
That sounds very insightful and meaningful, but is it remotely true? I can’t think of a single instance of its being true.
Before Bill Gates and Steve Jobs, did the computer industry have a “shared goal that united the activities of all stakeholders?” What would that “shared goal” have been? Did the goal change when Microsoft and Apple came along? It would seem that the goal of these two companies was to eat IBM’s lunch. I doubt IBM shared that goal.
Ditto with every significant innovation, ever. The “shared goal” of existing stakeholders is to divvy up the market and keep out competitors. Is that really how performance and accountability are improved? The “shared goal” of new competitors is to get rid of the old “stakeholders” and persuade consumers that there are new and better ways to fulfill their needs.
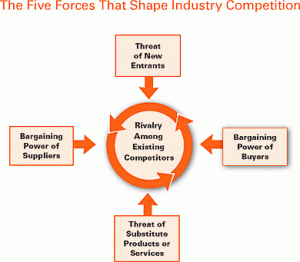
Porter actually knows this. In 2008 the Harvard Business Review published an update of Porter’s “Five Forces” analysis of competitive dynamics that included his famous graphic –
Where is the “shared goal that unites the interests and activities of all stakeholders” in this?
Porter’s NEJM article goes on with some useful suggestions but an awful lot of platitudes. For instance, he says that health care should be based on value to the patient, “value” being defined as “outcomes relative to costs.” Then he writes –
Outcomes, the numerator of the value equation, are inherently condition-specific and multidimensional. For any medical condition, no single outcome captures the results of care.
But a “numerator” is by definition a number. How can we develop a single number to represent outcomes when they are so “multidimensional” and “condition specific?”
In fact, I would argue that the whole idea that “value to the patient” can be defined objectively is misguided. Even with precisely the same cost and the same medical outcome, the “value” of a service will be different for every patient. Dick Cheney seems to be very happy with his heart transplant and thrilled to extend his life by several more years. Someone else might think that the ordeal of the surgery and medical attention isn’t worth it. Or they might think that their life is pretty crappy and not worth extending.
This doesn’t apply just to health care. The value of a new Mercedes is different for you and me. You might think having such a car is proof to the world that you have arrived: it shows how successful and prosperous you are. I might be embarrassed by the conspicuous consumption and prefer something more modest. I might prefer to spend the money on charitable contributions. The difference is entirely subjective.
The balance of Porter’s article illustrates how futile his quest is. Some quotes –
- Because care activities are interdependent, value for patients is often revealed only over time and is manifested in longer-term outcomes such as sustainable recovery, need for ongoing interventions, or occurrences of treatment-induced illnesses
- For patients with multiple medical conditions, value should be measured for each condition, with the presence of the other conditions used for risk adjustment.
- The concept of quality has itself become a source of confusion.
- No organization I know of systematically measures the entire outcome hierarchy for the medical conditions for which it provides services
- Current cost-measurement approaches have also obscured value in health care and led to cost- containment efforts that are incremental, ineffective, and some-times even counterproductive.
Whew! What a great number of windmills for this Don Quixote to attack!


The whole problem with any of this is that the value of a service or product is what is defined by the buyer. Mercedes’ are nice to look at, but I wouldn’t have one, even if I could afford it. My 5-year old Honda does just fine.
Some patients want to be totally fixed, others just want to be a little better. Some patients can only be fixed just so much.
This whole “value-based” argument is brought on because we have third parties paying for healthcare, and they want to save money, so we establish parameters,benchmarks, goals, etc for the doctor and the patient. If either one or both are not hitting the mark, the doc may not get paid. Maybe the patient doesn’t want to or can’t hit that mark.
It’s an artificial system. If I am not satisfied with the work by my accountant, attorney, plumber, mechanic, I go somewhere else. If my mechanic says I need new brakes but I can’t afford it then, I put it off until I can, but I still pay him for looking, and the brakes are now my responsibility. I don'[t know of any other payment system that makes these kind of value judgements outside of the consumer-provider relationship.
I agree Perry. Anytime 3rd parties get involved, inefficiencies pop up. That is because not only do the patient and healthcare worker have to be satisfied, but now a third party, or even a fourth party, have to also be satisfied. Whenever that happens, prices rise, choices shrink, and deadweight loss is incurred.
Nothing is ‘borne out’ by any of this at this stage. We are on the first few miles of a journey, not the last mile.
What new system or process do you know of that, when it began didn’t create additional work? Those that were successful, people would be hard pressed to give up a year or two later.
The articles in the early days of any change that report on things not working, not yielding results and so forth are simply pieces to fill copy in my view. They are written without reliable facts borne out over time.
Ford Motor Company thought they could make the Edsel work. Sure, it had all kinds of technical problems with a silly transmission selector in the steering wheel and an ugly grill, among other things. They “fixed” most of these problems in the next two model years but they failed. Why? The public didn’t want the car.
The same thing applies to centralized healthcare management. It is a bad idea to begin with, and no amount of tweaking is going to change that fact.
To paraphrase a misquotation of Oscar Wilde: The problem with health care is too many meetings.
I have met entrepreneurs who would succeed in other industries where they do not have to get the permission of all the stakeholders before they act. In health care, government tends to hinder their action because what they propose as a business does not fix the whole system.
Before Bill Gates and Steve Jobs, did the computer industry have a “shared goal that united the activities of all stakeholders?” It would seem that the goal of these two companies was to eat IBM’s lunch. I doubt IBM shared that goal.
Greg, that’s an interesting observation. If there’s one thing I’ve noticed about academic and bureaucratic elites in health care, it’s that they assume there are “shared goals” that all stakeholders are willing to pursue — even when it’s not in the stakeholders’ self-interest to do so.
In health care who are the stakeholders? Presumably, they are patients, doctors, insurers, government payers, hospitals, employers, and the allied staff and associated suppliers.
Do these stakeholders have a shared goal? In fact, the stakeholders’ goals aren’t shared — their constantly at odds. Providers want to maximize revenue against reimbursement formulas. Patients want medical care until it’s only worth what they pay at the margin. Insurers want to pay out as little of their premiums in claims as is reasonable possible. Medical suppliers want their products used — even if they’re of little benefit. Public health advocates want all the stakeholders to subsidize care for the poor and elderly.
This is all part of a government takeover of medicine and utterly insane. I am a physician running for Congress. If you want to stop this, help me get elected and donate to my campaign at http://www.macfarlane2014.com.
Regards
You are a certified buzz-kill, Greg. I just came back from the patent office where I had registered a brand-new concept named “Value Valuing.” My ideas was to market this concept to various conference organizers for panel discussions. Just think of it, dividing vectors by one number or vice versa would be completely incomprehensible to the audience, but with enough math and new ‘cetps I could come across as a savvy visionary.
And now this!
Don’t worry, Uwe, there will always be a market for dumb ideas with high falutin’ titles or scary premises.
I had dinner with a friend on Saturday, someone I don’t get to see that often. He was explaining to me his new diet. He said that all the prior concerns about eating fat were wrong and the real problem is eating sugar, including fruit. Good grief! The same people who told us with absolute certainty that eating fat was bad are now telling us with absolute certainty that eating sugar is bad.
In ten years we will discover that eating fruit was a pretty good idea all along. Meanwhile, lots of people will make lots of money scaring the bejeebers out of the gullible.
Yes, which is why I eat butter. It is a negatively lagged response to the discovery, coming out in late 2017, that butter is good for you.
Professor Reinhardt, don’t abandon your dream so easily! I think it’s a brilliant idea!
First you need to write a textbook on Value Valuing (not to be confused with “Valuing Value,” which is obviously just a bunch of meaningless jargon). Then you force your students to use the text book in your classes. As your students graduate, and go out into the health care world, they create a lot of buzz about this novel idea.
Once you release your second edition of Value Valuing, you hit lecture circuit, you get paid to keynote conferences and participate in panel discussions.
Because it’s self-evident that all us health policy wonks should learn to value value, you could become the new darling of the health policy rhetoric world!
Only in health care would such a scheme work!
You can’t interpret this ratio outcome/costs literally as meaning “value” in health care. All you have to do is to allow outcomes to go down the toilet, but not charge as much in proportion. . You therefore have a high ratio, which equals value, because the denominator is approaching zero. This becomes a silly result.
The value in health care has to have some relationship with the absolute value of the outcome, No.matter what the costs, the outcome has to be getting better, year after year, bit by bit. A reduced cost can amplify or augment this value but we should not tolerate an outcome that gradually becomes inferior to that of what medical science can offer today. Otherwise, we betray science and beneficence.
The Hippocratic Oath doesn’t mention costs. This use of the concept of value allows providers to reduce their efforts, and hence accept shabby outcomes, as long as costs are proportionately decreased more. This is easy: we nearly stop doing something expensive and we completely stop charging for it. This gives us an A in value, but it causes health care to degenerate into a vocation that none of us would respect.
The mischief of dividing by zero.
You raise an interesting point. The consensus in health care seems to be “costs be damned,” — do whatever it takes regardless of costs.
The problem is that we could — at least in theory — spend our entire GDP on health care. As an economist, I believe it is self-evident that some trade-offs must be made. The only question is: who should make the trade-off choices? Should it be doctors, bureaucrats or patients themselves?
Presumably, if government or third-party payers are paying the cost, you seem to suggest any improvement in outcome (no matter how small) is your Hippocratic Oath. Yet if patients themselves are paying the bill directly, we know that the trade-offs will occur much sooner — if for no other reason that what economists call the Budget Constraint.
You are correct that to some degree there is a relationship between spending and outcomes. But we still need to define value as the optimal trade-off between exhausting the last resource achieving the best possible outcome and efficient care.
In the example of the CalPERS/WellPoint experiment with value-based care in California, there was no identifiable difference in care quality. There was, however, a big difference in the average price charged for joint replacement among enrollees before and after the experiment began.
@Herrick
You don’t want a reduction in costs to improve value if outcomes are also becoming worse but at a slower rate. The absolute value of the numerator should be protected for value to have meaning.
As you know, most chemo offers only months added lifespan (although some is curative). Stop most chemo, charge even less, and we show value gains. Similar exercises can be found elsewhere in health care. Do we want these changes?
My point is that we shouldn’t literally believe that value equals outcomes/costs, but should favor the outcomes, and seek to keep them at least stabile or slightly improving over time.
We should not denigrate outcomes because we revere value.